Smoking is a well-known risk factor for a variety of diseases, and recent evidence suggests that it has a detrimental effect on periodontal health. However, the exact relationship between smoking and periodontal disease is not yet fully understood. Smoking can cause defects in neutrophil function, alter inflammatory and immune responses to periodontal pathogens, and have both systemic and local effects. Studies have shown that smoking is associated with an increased rate of periodontal disease, including alveolar bone loss, loss of adhesion, and pocket formation.
Nicotine
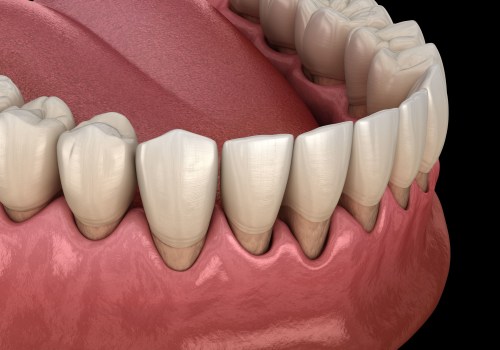
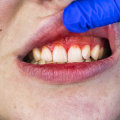
, the main component of cigarette smoke, can weaken the body's defenses against bacterial invasion caused by plaque.It has been observed that the use of metronidazole and amoxicillin systemically in the SRP treatment of smokers with chronic periodontitis can reduce the average counts and proportions of periodontal pathogens, such as Treponema. Additionally, some periodontal pathogens can subvert the host's immune response, forming a vicious cycle. The association between periodontal disease and oral neoplasms may be explained indirectly by the possibility that a breach in the mucosal barrier caused by periodontal disease allows carcinogens such as tobacco and alcohol to penetrate. This phenomenon is known as masking of the disease because the vasoconstrictive properties of tobacco smoke can hide the inflammatory and destructive changes that occur in the periodontium (see figures 1a and 1b). In vitro studies have shown that both gingival fibroblasts (HGF) and periodontal ligament fibroblasts (PDLF) have reduced cell viability when exposed to increasing concentrations of cigarette smoke extract (CSE) and nicotine. The susceptibility to periodontal disease varies depending on an individual's bacterial flora and specific local and systemic factors.
In vitro studies have also demonstrated that nicotine can inhibit the growth of gingival fibroblasts and reduce the production of fibronectin and collagen, which are essential for healthy periodontium. Lower concentrations of CSE may promote biofilm formation in bacteria-related periodontal disease and cause a stress reaction, thus acting as an environmental modulator of bacterial metabolism and survival. Since smokers have different etiologies and clinical manifestations of periodontal disease compared to non-smokers, they also respond differently to periodontal treatment. Other effects of smoking include decreased blood flow and impaired revascularization of periodontal tissues, leading to delayed wound healing. These expenses include dental expenses, as smoking increases the progression of the disease and complicates its treatment.